Dental Implant Abutments: Types, Materials and How They Work
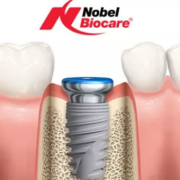
A dental implant abutment is the connector piece that joins the titanium implant post — which is fixed in the jawbone — to the visible crown, bridge or prosthesis on top. Without the abutment, the implant and the restoration cannot be joined. Understanding what abutments are and how they work helps patients make sense of their treatment plan and the components involved in their restoration.
At Asensio Advanced Dentistry in Valencia, abutment selection is part of the treatment planning process for every implant case. The choice of abutment type and material affects the fit, aesthetics and long-term stability of the final restoration. Dr. Lucía Asensio Romero, specialist in implantology and oral surgery with over 30 years of experience, selects the appropriate abutment for each case based on the implant system, bone level, gum tissue and prosthetic design.
The three components of a dental implant
A complete dental implant restoration consists of three distinct components, each with a specific function:
| Component | Location | Function |
|---|---|---|
| Implant fixture | Inside the jawbone | Replaces the tooth root — titanium post that fuses with bone through osseointegration |
| Abutment | At gum level | Connects the implant fixture to the crown — provides the shape the crown sits on |
| Crown / prosthesis | Above the gum | The visible restoration — designed to match surrounding teeth in colour, shape and function |
Types of dental implant abutments
Different stages of treatment require different abutment types. The three main categories are:
| Type | When used | Purpose |
|---|---|---|
| Healing abutment | Immediately after implant placement | Shapes the gum tissue around the implant while osseointegration occurs — removed before final restoration |
| Temporary abutment | During osseointegration period | Supports the provisional crown while the implant integrates — replaced at second visit |
| Final abutment | At second visit after osseointegration | Permanent connector for the definitive crown — precision-fit to the specific implant and crown design |
Abutment materials
The choice of abutment material affects both the aesthetics and the mechanical performance of the restoration. The most commonly used materials are:
| Material | Advantages | Best used for |
|---|---|---|
| Titanium | Maximum strength, biocompatible, lightweight, long clinical track record | Most cases — the default choice for strength and reliability |
| Zirconia | Tooth-coloured — eliminates grey gum line, excellent biocompatibility | Front teeth where aesthetics are critical and gum tissue is thin |
| Gold alloy | Excellent precision fit, biocompatible | Complex prosthetic cases requiring precision casting |
| PEEK (polyether ether ketone) | Lightweight, tooth-coloured, used for temporaries | Provisional restorations during osseointegration |
At Asensio, abutments are sourced exclusively from Nobel Biocare and Klockner — the same implant brands used for the fixtures. Using manufacturer-matched components ensures precise fit, consistent performance and compatibility with the lifetime guarantee on materials.
Frequently asked questions
Is the abutment included in the implant price?
Yes. At Asensio, the quoted price for a single implant (£850) includes the implant fixture, abutment and porcelain crown — all three components. There are no hidden additions for standard cases. View the full breakdown on our prices page.
Can an abutment fail or need replacing?
Abutment loosening is one of the most common minor implant complications. It is usually resolved by retightening or replacing the abutment — a straightforward procedure that does not affect the implant fixture itself. If you experience a loose or uncomfortable crown, contact us promptly rather than leaving it, as a loose abutment can cause damage to the implant connection over time.
What is the difference between a cement-retained and a screw-retained crown?
Crowns can be attached to abutments either by dental cement or by a small retaining screw. Screw-retained crowns are removable by the dentist for maintenance or adjustment — they are generally preferred for implant restorations because they allow easier access if the abutment needs attention. Cement-retained crowns are fixed permanently and cannot be removed without risk of damage.
Do I need to do anything special to care for my abutment?
The abutment itself requires no special care beyond the standard implant cleaning routine — soft toothbrush, interdental brush and water flosser daily. The critical area to clean is the junction between the abutment and the gum, where bacterial biofilm accumulates and can cause peri-implant infection if not removed regularly. See our dental implant care guide for full instructions.
Related guides
- Dental implants abroad at Asensio — full overview of implant treatments for UK patients
- Osseointegration — how the implant fixture bonds with the bone
- Types of dental implants — which solution is right for your case
- Fixed dental prosthesis cost — prices and options for fixed restorations
- Care of dental implants — daily routine and professional review guide
- Peri-implantitis — the main risk to long-term implant success